
Thursday, April 16, 2020 - 10:00
Maynooth University and Trinity College collaborate on major Irish Covid-19 study
Researchers from Ireland (Maynooth University and the Centre for Global Health, Trinity College Dublin), Northern Ireland (Ulster University), Scotland (Edinburgh Napier University), and England (University of Sheffield) have released the first wave of the Irish COVID-19 Psychological Survey; a multi-wave study running throughout the COVID-19 outbreak to better understand how people are responding, understanding, and coping with the pandemic.
Over 1,000 adult citizens of the Republic of Ireland completed the survey, which was launched on 31 March; 31 days after the first confirmed case of COVID-19 was reported in the Republic of Ireland. The survey was launched 19 days after An Taoiseach Leo Varadkar announced sweeping restrictions on the movement of people, and two days after Irish residents were required to stay at home. Participants answered questions about their current circumstances of the COVID-19 pandemic, their mental health, and their views on COVID-19 vaccination.
Initial results suggest that mental health problems are common; 41% of people reported feeling lonely, 23% reported clinically meaningful levels of depression, 20% reported clinically meaningful levels of anxiety, and 18% reported clinically meaningful levels of post-traumatic stress.
Dr Philip Hyland of Maynooth University, said of the results: “We’re seeing high rates of mental health problems like depression, anxiety, and post-traumatic stress, and these problems are affecting men and women differently. Women are experiencing higher levels of depression and anxiety whereas men are experiencing higher rates of post-traumatic stress.” Dr Hyland added that “almost half of the people surveyed were feeling lonely and those people with higher levels of loneliness were most likely to experience adverse mental health problems. We also found that younger people, those who have a tendency to think in catastrophic ways, those who fear being infected by COVID-19, and those who have had someone close to them infected by COVID-19 are at a higher risk of mental health problems.”
Dr Frédérique Vallières, Director of Trinity College’s Centre for Global Health further added: “Despite encouraging results in terms of people’s knowledge on COVID-19, we further found that attitudes towards the uptake of a potential COVID-19 vaccine to be worryingly low, with only 65% of people indicating that they would accept a vaccine for themselves and their children. One-in-four people did say however that they might accept a vaccine for themselves and their child, compared to one-in-ten people who said they would not. A better understanding of why people might be hesitant to accept a COVID-19 vaccine, if and when it is developed is required.”
The second wave of the COVID-19 Psychological Survey is scheduled to commence prior to the 5 May. The research team will examine what effect prolonged quarantine and physical distancing measures have on people’s mental health and wellbeing, and what can be done to safeguard the mental health of the nation during this and any future health emergency. The research team seek to understand more about COVID-19 vaccine hesitancy.
Speaking about the importance of the survey, Dr Philip Hyland added: “The social and political context of the present crisis is unique and the mental health consequences of this pandemic need to be properly understood to ensure the nation’s swift return to normal functioning when it is safe to do so.”
The research team are currently preparing multiple scientific papers and will release these findings as soon as possible. The findings of this next wave of the study will be delivered next month.
There are a number of helplines available for anyone who is affected by issues of stress, including those below:
Turn2me: www.Turn2me.ie
SpunOut.ie: SpunOut.ie is Ireland's youth information website by young people, for young people. Funded by the HSE. www.SpunOut.ie
Pieta House: 1800 247 247. TXT Helpline: 51444 www.pieta.ie
Health Service Executive: The HSE website has updated factual information and advice regarding COVID-19 (coronavirus) HSE.ie. If you develop a fever or any respiratory symptoms contact your GP or HSELive on 1850 241 850.
RESEARCH TEAM
Maynooth University
- Dr Philip Hyland, Associate Professor of Psychology,
Trinity College Dublin
- Dr Frédérique Vallières, Director of the Trinity Centre for Global Health,
Ulster University
- Professor Mark Shevlin, Professor of Psychology
- Professor Jamie Murphy, Professor of Psychology
- Dr Orla McBride, Reader in Psychology
Edinburgh Napier University
- Professor Thanos Karatzias, Professor of Mental Health
University of Sheffield
- Professor Richard Bentall, Professor of Clinical Psychology
1. How many people are suffering from a mental health problem in Ireland?
The survey used standardised measures of loneliness1, major depression2, generalized anxiety disorder3, and post-traumatic stress responses4. Standard cut-off scores were applied to identify participants whose responses were indicative of clinically meaningful levels of mental health problems.
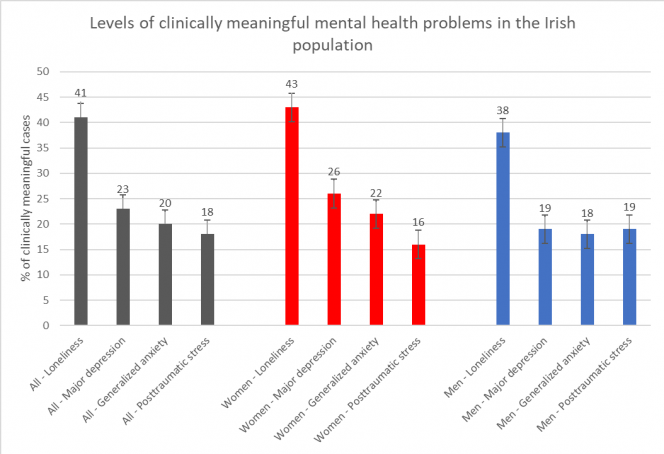

Comment:
- More than four-in-ten Irish adults are currently feeling lonely.
- Nearly one-in-four Irish people are experiencing clinically meaningful levels of depression, and one-in-five are experiencing anxiety and post-traumatic stress problems.
- More women than men are experiencing clinically meaningful levels of loneliness, depression, and anxiety.
- More men than women are experiencing clinically meaningful levels of post-traumatic stress problems.
Hughes, M.E., Waite, L.J., Hawkley, L.J., & Cacioppo, J.T. (2004). A short scale for measuring loneliness in large surveys:
Results from two population-based studies. Research on Aging, 26, 655-672.
2Kroenke, K., Spitzer, R. L., & Williams, J. B. (2001). The PHQ-9: validity of a brief depression severity measure. Journal of General Internal Medicine, 16(9), 606–613. https://doi.org/10.1046/ j.1525-1497.2001.016009606.x
3Spitzer, R. L., Kroenke, K., Williams, J. B., & Löwe, B. (2006). A brief measure for assessing generalized anxiety disorder: the GAD-7. Archives of Internal Medicine, 166(10), 1092-1097. doi: 10.1001/archinte. 166.10.1092. 4Cloitre, M., Shevlin, M., Brewin, C. R., Bisson, J. I., Roberts, N. P., Maercker, A., ... & Hyland, P. (2018). The International Trauma Questionnaire: development of a self‐report measure of ICD‐11 PTSD and complex PTSD. Acta Psychiatrica Scandinavica, 138(6), 536-546. doi: 10.1111/acps.12956.
2. Who are most vulnerable to having a mental health problem?
People who screened positive for a clinically significant mental health problem – depression, generalized anxiety, or post-traumatic stress problems - were compared across 22 risk factors including demographic, occupational, political, financial, physical health, and psychological variables.
Screening positive for a mental health problem was significantly associated with (in this order of strength):
- Higher levels of loneliness
- Younger age
- Higher levels of catastrophic thinking (‘I turn minor issues into really big problems in my head’)
- Higher perceived risk of COVID-19 infection in the next month
- A loved one having been infected by COVID-19
Comment: Having a mental health problem is associated with psychological (loneliness, catastrophizing, fear of COVID-19 infection) and personal (age and knowing someone who has been infected by COVID-19) factors.
3. Attitudes towards COVID-19 vaccination.
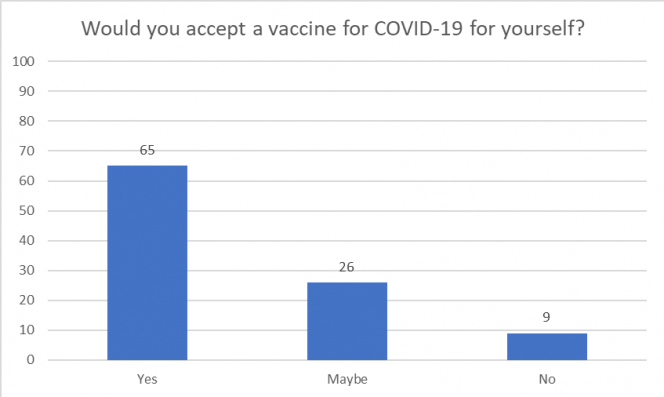

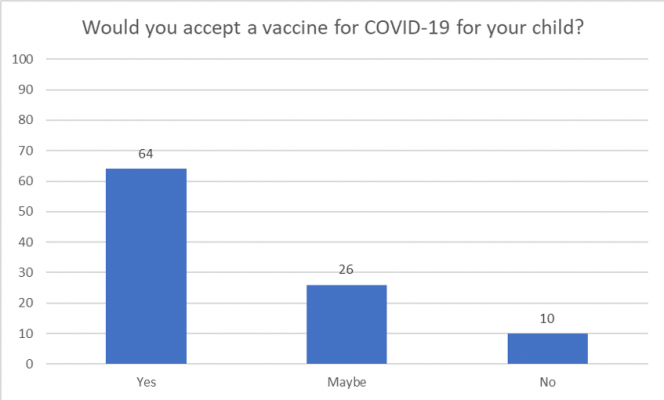
Comment:
- Just two-thirds of people said they would accept a vaccine to prevent COVID-19 for themselves and for their child.
- One-in-four people said they might accept a vaccine for themselves and their child.
- One-in-ten people said they would not accept a vaccine for themselves and their child.
SUMMARY
The picture that has emerged from this study is that many people in the Irish population are currently experiencing mental health problems. Just under half of the participants reported feeling lonely, and 35% of people had levels of depression, anxiety, or post-traumatic stress that are indicative of a need for clinical care. An extensive array of risk factors for having a mental health problem were investigated and the most important risk factor was loneliness.
We found worryingly low levels of willingness to accept a vaccine for COVID-19 if one were to be developed. Approximately one-third of people did not say that they would accept a vaccine for themselves or their child. If a vaccine is developed, the rate of uptake will likely need to be higher than this for it to be effective against COVID-19.
